$24.00
Description
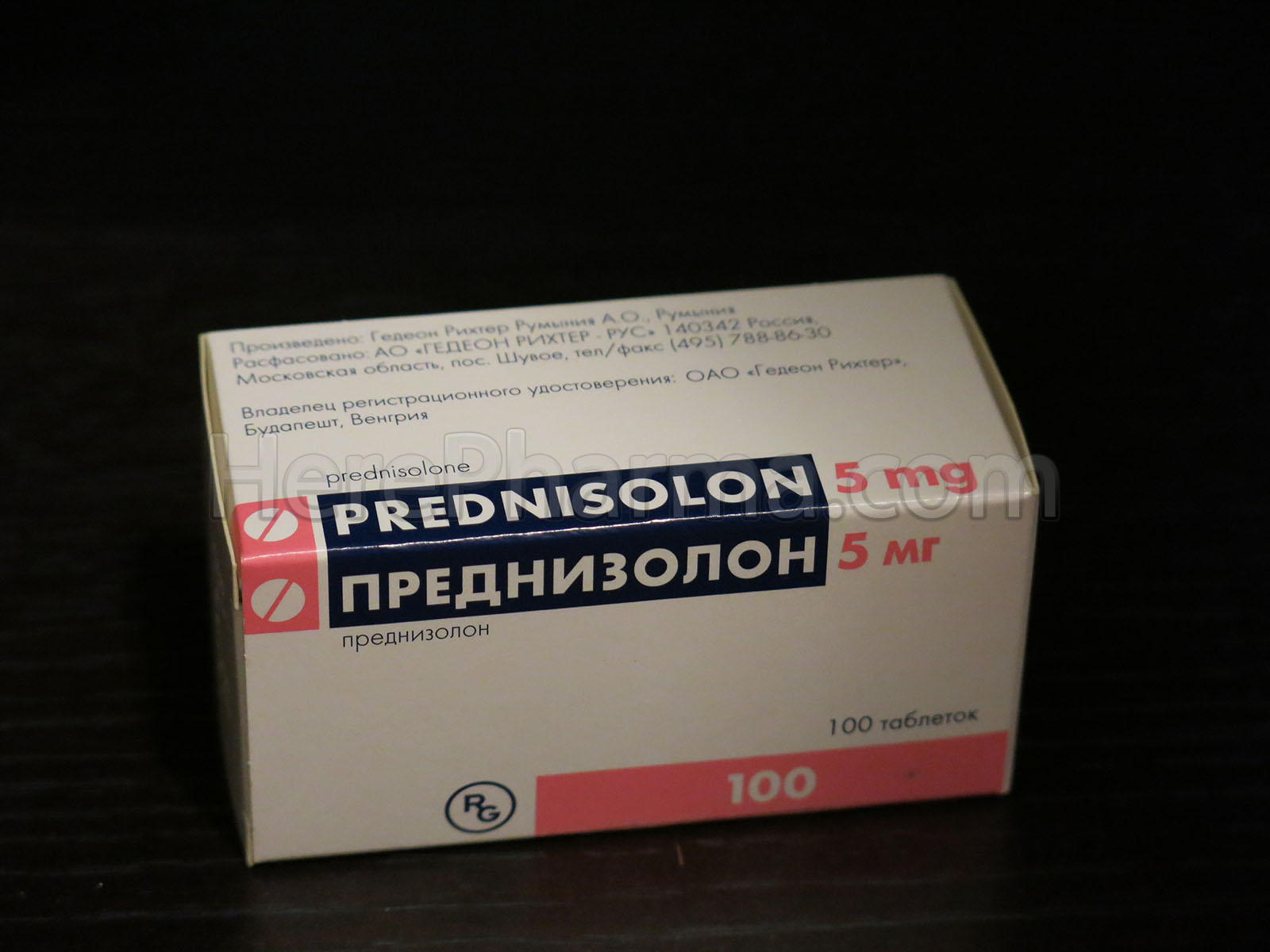
Prednisolon 5mg 100 tablets
Product form, composition and packaging
Tablets 1 tab.
prednisolone 5 mg
Excipients: lactose, corn starch, silicon colloidal dioxide, stearic acid, sodium carboxymethyl starch, magnesium stearate.
Pharmacological action
GKS. Inhibits the function of leukocytes and tissue macrophages. Limits the migration of leukocytes to the area of inflammation. It violates the ability of macrophages to phagocytosis, as well as to the formation of interleukin-1. It helps to stabilize the lysosomal membranes, thereby reducing the concentration of proteolytic enzymes in the area of inflammation. Decreases capillary permeability caused by histamine release. Inhibits the activity of fibroblasts and collagen formation.
Inhibits the activity of phospholipase A2, which leads to the suppression of the synthesis of prostaglandins and leukotrienes. Inhibits the release of COX (mainly COX-2), which also helps to reduce the production of prostaglandins.
Reduces the number of circulating lymphocytes (T – and B-cells), monocytes, eosinophils and basophils due to their movement from the vascular bed to lymphoid tissue; suppresses the formation of antibodies.
Prednisolone inhibits pituitary release of ACTH and β-lipotropin, but does not reduce the level of circulating β-endorphin. It inhibits secretion of TSH and FSH.
With direct application to the vessels of has vasoconstrictor effects.
Prednisolone has a pronounced dose-dependent effect on the metabolism of carbohydrates, proteins and fats. It stimulates gluconeogenesis, promotes the capture of amino acids by the liver and kidneys and increases the activity of gluconeogenesis enzymes. In the liver, prednisolone enhances the deposition of glycogen by stimulating the activity of glycogen and synthesis of glucose from the products of protein metabolism. The increase in the concentration of blood glucose activates the secretion of insulin.
Prednisone suppresses the seizure of glucose by fat cells that leads to activation of lipolysis. However, due to increased insulin secretion, lipogenesis is stimulated, which contributes to the accumulation of fat.
It has a catabolic effect in lymphoid and connective tissue, muscles, adipose tissue, skin, bone tissue. To a lesser extent than hydrocortisone, affects the processes of water-electrolyte metabolism: promotes the excretion of potassium and calcium ions, delay in the body of sodium ions and water. Osteoporosis and Cushing’s syndrome are the main factors limiting long-term therapy of GCS. The result of the catabolic actions may suppress growth in children.
In high doses prednisone can increase the excitability of brain tissue and contributes to lowering the threshold of convulsive readiness. It stimulates the excess production of hydrochloric acid and pepsin in the stomach, which leads to the development of peptic ulcer.
In systemic use, the therapeutic activity of prednisolone is due to anti-inflammatory, antiallergic, immunosuppressive and antiproliferative effects.
With external and local application, the therapeutic activity of prednisolone is due to anti-inflammatory, anti-allergic and anti-exudative (due to the vasoconstrictor effect) action.
Compared with hydrocortisone, the anti-inflammatory activity of prednisolone is 4 times more, the mineralocorticoid activity is 0.6 times less.
Pharmacokinetics
When ingestion is well absorbed from the gastrointestinal tract. Cmax in plasma observed after 90 min In the plasma most of prednisolone is associated with transcortin (corticospinalis globulin). It is metabolized mainly in the liver.
T1/2 is about 200 min. Excreted by the kidneys unchanged to 20%.
Indications
For oral and parenteral use: rheumatism; rheumatoid arthritis, dermatomyositis, periarteritis nodosa, scleroderma, ankylosing spondylitis, bronchial asthma, status asthmaticus, acute and chronic allergic diseases, anaphylactic shock, Addison’s disease, acute adrenal insufficiency, adrenogenital syndrome; hepatitis, hepatic coma, gipoglikemicakie state, lipoid nephrosis; agranulocytosis, various forms of leukemia, Hodgkin’s disease, thrombocytopenic purpura, haemolytic anaemia; small chorea; pemphigus, eczema, itching, exfoliative dermatitis, psoriasis, pruritus, seborrheic dermatitis, SLE, erythroderma, alopecia.
For intraarticular administration: chronic polyarthritis, post-traumatic arthritis, osteoarthritis of large joints, rheumatic lesions of individual joints, arthrosis.
For infiltration into tissues: epicondylitis, tenosynovitis, bursitis, shoulder periarthritis, keloids, ischialgia, Dupuytren’s contracture, rheumatic and similar lesions of the joints and various tissues.
For use in ophthalmology: allergic, chronic and atypical conjunctivitis and blepharitis; inflammation of the cornea with intact mucosa; acute and chronic inflammation of the anterior segment of the choroid, sclera and episclera; sympathetic inflammation of the eyeball; after injuries and operations with prolonged irritation of the eyeballs.
For use in gynecology: treatment of vaginitis (as part of combination therapy with antibiotics and antifungal agents).
Dosage regimen
When administered for replacement therapy in adults, the initial dose is 20-30 mg/day, supporting dose – 5-10 mg / day. If necessary, the initial dose may be 15-100 mg/day, supporting – 5-15 mg / day. The daily dose should be reduced gradually. For children, the initial dose is 1-2 mg/kg/day in 4-6 doses, supporting – 300-600 mg/kg / day.
When/m or/in the dose, the multiplicity and duration of application are determined individually.
When intra-articular administration in large joints, a dose of 25-50 mg is used, for medium – sized joints – 10-25 mg, for small joints-5-10 mg. for infiltration into the tissues, depending on the severity of the disease and the size of the affected area, doses from 5 to 50 mg are used.
Locally in ophthalmology used 3 times/day, the course of treatment – no more than 14 days; in dermatology – 1-3 times / day.
Locally in gynecology-as part of combined drugs with antibiotics and antifungal agents in accordance with the recommended dosage regimen.
Contraindications to use
For short – term use for vital signs-hypersensitivity to prednisolone.
For intra-articular administration and introduction directly into the lesion: previous arthroplasty, pathological bleeding (endogenous or caused by the use of anticoagulants), intra-articular bone fracture, infectious (septic) inflammatory process in the joint and periarticular infections (incl. in history), as well as a General infectious disease, pronounced periarticular osteoporosis, lack of signs of inflammation in the joint (“dry” joint, for example, osteoarthritis without synovitis), severe bone destruction and joint deformation (sharp narrowing of the articular gap, ankylosis), joint instability as the outcome of arthritis, aseptic necrosis of bone epiphyses forming the joint.
For external use: bacterial, viral, fungal skin diseases, skin tuberculosis, skin manifestations of syphilis, skin tumors, post – vaccination period, violation of the integrity of the skin (ulcers, wounds), childhood (up to 2 years, with itching in the anus-up to 12 years), rosacea, vulgar acne, perioral dermatitis.
For use in ophthalmology: bacterial, viral, fungal eye diseases, tuberculosis eye damage, trachoma, violation of the integrity of the eye epithelium.